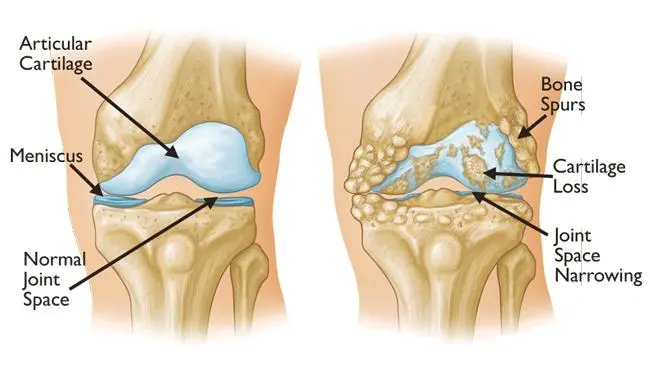
Osteoarthritis (OA): What You Need to Know Osteoarthritis (OA) is the most common chronic joint condition. It is also known as wear-and-tear arthritis or degenerative joint disease. A joint is where two bones come together. The ends of these bones are covered by a protective tissue called cartilage. With OA, this cartilage breaks down, causing the bones within the joint to rub together. This leads to pain, stiffness, and other symptoms. OA can occur in any joint. However, the most commonly affected areas include: Hands Fingers Shoulders Spine (especially the neck and lower back) Hips Knees OA occurs mostly in older adults, although it can affect people of any age. It is a leading cause of disability. According to the Centers for Disease Control and Prevention (CDC), OA affects more than 32.5 million adults in the United States. Osteoarthritis Symptoms The most common symptoms of OA include: Joint pain Stiffness Inflammation Bone spurs (extra bone growth, usually painless) Tenderness when pressing on affected areas Crepitus (grating, cracking, clicking, or popping sounds when moving joints) What Causes Osteoarthritis? OA is caused by joint damage that builds up over time. This is why age is one of the main risk factors—the older you are, the more wear and tear your joints have experienced. Other causes of joint damage include: Past injuries (such as torn cartilage, dislocated joints, or ligament damage) Joint misalignment or malfunction Obesity (which increases pressure on joints) Having OA in one joint can also increase the risk of developing it in other parts of the body. Treatment for Osteoarthritis There is no cure for OA, so treatment focuses on managing symptoms and improving quality of life. In many cases, a combination of the following is effective: Over-the-counter (OTC) medications Lifestyle changes Home remedies OA is typically a progressive condition with stages ranging from 0 to 4: Stage 0: Normal joint Stage 4: Severe osteoarthritis However, not everyone progresses to the later stages. The condition often stabilizes before reaching severe levels. Medications Several types of medications can help relieve OA symptoms: Oral pain relievers to reduce discomfort Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen Corticosteroids (e.g., cortisone injections) Lifestyle Tips for Managing OA Simple daily habits can significantly improve symptoms and overall well-being: Engage in low-impact exercises like walking or swimming (about 30 minutes daily) Stretch regularly to maintain flexibility Get adequate sleep to reduce inflammation Maintain a healthy weight to reduce pressure on joints Avoid prolonged inactivity Osteoarthritis Prevention While some risk factors—such as age and genetics—cannot be changed, others can be managed. To reduce your risk: Maintain a healthy weight Stay physically active Protect your joints from injury Practice good posture and body mechanics Outlook and Summary Osteoarthritis is a chronic condition with no cure, but the outlook is positive with proper management. Do not ignore persistent joint pain or stiffness. The sooner you consult a rheumatologist, the sooner you can: Receive an accurate diagnosis Begin appropriate treatment Improve your quality of life
Gout Symptoms, Causes & Diet Recommendations
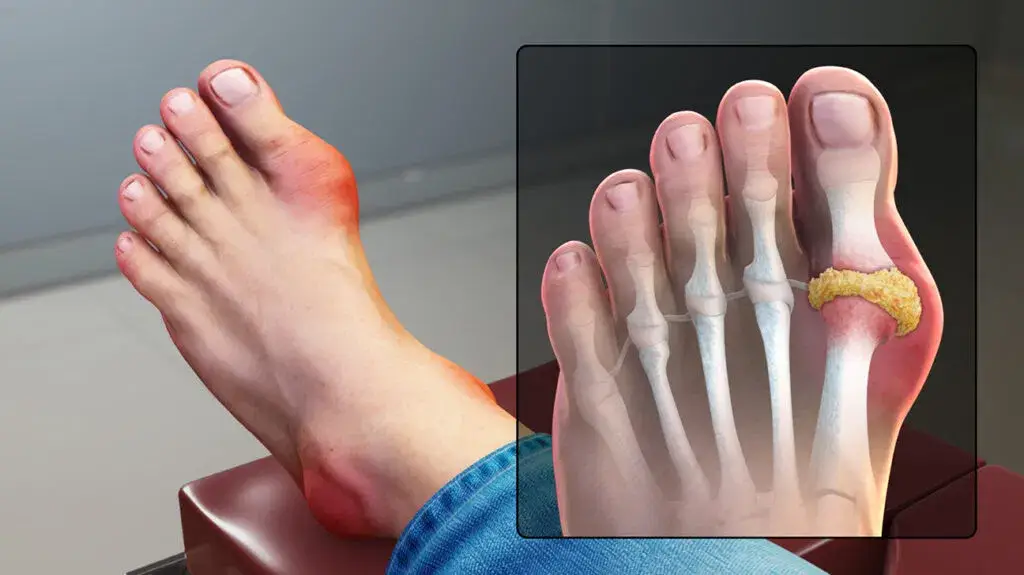
Gout is due to persistently elevated levels of uric acid in the blood This occurs from a combination of diet , other health problems , and genetic factors. At high levels, uric acid crystallizes and the crystals deposit in joints, tendons , and surrounding tissues , resulting in an attack of gout. Gout occurs more commonly in those who regularly drink beer or sugar-sweetened beverages or who eat foods that are high in purines such as liver, shellfish, or anchovies, or are overweight. Diagnosis of gout may be confirmed by the presence of crystals in the joint fluid or in a deposit outside the joint. Blood uric acid levels may be normal during an attack . Gout symptoms Gout can present in several ways, although the most common is a recurrent attack of acute inflammatory arthritis (a red, tender, hot, swollen joint). The joint at the base of the big toe is affected most often, accounting for half of cases. Other joints, such as the heels, knees, wrists, and fingers, may also be affected. Joint pain usually begins during the night and peaks within 24 hours of onset. This is mainly due to lower body temperature. Other symptoms may rarely occur along with the joint pain, including fatigue and a high fever. Long-standing elevated uric acid levels ( hyperuricemia ) may result in other symptoms, including hard, painless deposits of uric acid crystals known as tophi . Extensive tophi may lead to chronic arthritis due to bone erosion. Elevated levels of uric acid may also lead to crystals precipitating in the kidneys, resulting in stone formation and subsequent uric acid pile up . Cause The crystallization of uric acid , often related to relatively high levels in the blood, is the underlying cause of gout. This can occur because of diet, genetic predisposition, or underexcretion of urate , the salts of uric acid . Underexcretion of uric acid by the kidney is the primary cause of hyperuricemia in about 90% of cases, while overproduction is the cause in less than 10%. About 10% of people with hyperuricemia develop gout at some point in their lifetimes . Long-standing elevated uric acid levels ( hyperuricemia ) may result in other symptoms, including hard, painless deposits of uric acid crystals known as tophi . Extensive tophi may lead to chronic arthritis due to bone erosion. Elevated levels of uric acid may also lead to crystals precipitating in the kidneys, resulting in stone formation and subsequent uric acid pile up . Lifestyle Dietary causes account for about 12% of gout , and include a strong association with the consumption of alcohol, sugar-sweetened beverages, meat, and seafood. Among foods richest in purines yielding high amounts of uric acid are dried anchovies , shrimp, organ meat , dried mushrooms, seaweed and beer yeast . Chicken and potatoes also appear related. Other triggers include physical trauma and surgery . Diagnosis Gout may be diagnosed and treated without further investigations in someone with hyperuricemia and the classic acute arthritis of the base of the great toe (known as podagra). Synovial fluid analysis should be done if the diagnosis is in doubt. Plain X – rays are usually normal and are not useful for confirming a diagnosis of early gout. They may show signs of chronic gout such as bone erosion . A definitive diagnosis of gout is based upon the identification of crystals in synovial fluid or a tophus . Prevention Risk of gout attacks can be lowered by complete abstinence from drinking alcoholic beverages , reducing the intake of fructose (e.g. high fructose corn – syrup) and purine – rich foods of animal origin, such as organ meats and seafood . Eating dairy products ,vitamin c – rich foods, coffee , and cherries may help prevent gout attacks, as does losing weight. Gout may be secondary to sleep apnea via the release of purines from oxygen-starved cells. Treatment of apnea can lessen the occurrence of attacks. Treatment The initial aim of treatment is to settle the symptoms of an acute attack. Repeated attacks can be prevented by medications that reduce serum uric acid levels. Tentative evidence supports the application of ice for 20 to 30 minutes several times a day to decrease pain . Options for acute treatment include non steroidal anti inflammatory drugs (NSAIDs), colchine ,and Glucocorticoids. While glucocorticoids and NSAIDs work equally well, glucocorticoids may be safer. Options for prevention include allopurinol , febuxostat , and probenecid. Lowering uric acid levels can cure the disease. Treatment of associated health problems is also important. Lifestyle interventions have been poorly studied. It is unclear whether dietary supplements have an effect in people with gout. NSAIDs NSAIDs are the usual first-line treatment for gout. No specific agent is significantly more or less effective than any other . Improvement may be seen within four hours and treatment is recommended for one to two weeks. They are not recommended for those with certain other health problems, such as gastrointestinal bleeding , kidney or heart failure. While indometacin has historically been the most commonly used NSAID, an alternative, such as ibuprofen , may be preferred due to its better side effect profile in the absence of superior effectiveness. For those at risk of gastric side effects from NSAIDs, an additional proton pump inhibitor may be given. Colchicine Colchine is an alternative for those unable to tolerate NSAIDs . At high doses, side effects (primarily gastrointestinal upset) limit its usage. At lower doses, which are still effective, it is well tolerated. Glucocorticoids Glucocorticoids have been found to be as effective as NSAIDs and may be used if contraindications exist for NSAIDs. They also lead to improvement when injected into the joint . Prognosis Without treatment, an acute attack of gout usually resolves in five to seven days; however, 60% of people have a second attack within one year. Those with gout are at increased risk of hypertension , diabetes mellitus , metabolic syndrome , and kidney and cardiovascular disease and thus are at increased risk of death. It is unclear whether medications that lower urate affect cardiovascular disease risks. This may be partly due to its association with insulin resistance and obesity, but some of the increased risk appears to be independent.
Lupus: Symptoms, Causes, Types & Treatments.
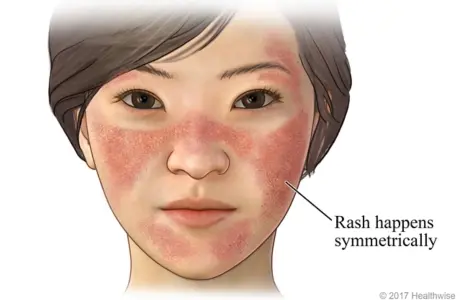
Lupus: What You Need to Know Lupus is an autoimmune condition in which the body’s immune system mistakenly attacks healthy cells and tissues. It can cause pain, inflammation, and complications across multiple organs and systems. These effects can range from mild to life-threatening. Systemic lupus erythematosus (SLE) is the most common form and can affect virtually any part of the body, including the skin, major organs, hair, muscles, joints, and digestive system. Who Does Lupus Affect? Most people with lupus are diagnosed between the ages of 15 and 44. According to the Lupus Foundation of America, lupus is most prevalent among women of childbearing age and is two to three times more common among women of color. Symptoms of Lupus Lupus symptoms can be subtle at first and may worsen over time. Common signs to watch for include: A butterfly-shaped rash across the cheeks and nose Chronic fatigue Unexplained fever Joint pain and persistent muscle aches Hair loss (alopecia) Swelling in the hands and feet Chest pain when taking deep breaths Types of Lupus There are several forms of lupus, including: Systemic lupus erythematosus (SLE) – affects the whole body Cutaneous lupus – primarily affects the skin Neonatal lupus – a rare condition affecting newborns Diagnosis There is no single test that can diagnose lupus. A rheumatologist typically evaluates a combination of symptoms, medical history, and laboratory tests to identify signs of systemic inflammation and immune system activity. Treatment Managing lupus requires a personalized treatment plan developed with a healthcare professional. Treatment options may include: Medications to control inflammation and immune response Lifestyle adjustments In some cases, complementary therapies such as acupuncture Managing the Condition Living with lupus can be challenging. Chronic pain and fatigue can be debilitating, often affecting daily activities and productivity. In some cases, access to treatment may also be a challenge. However, with the right care and support, many people are able to manage symptoms effectively and maintain a good quality of life. Summary If left untreated, lupus can lead to serious complications over time. Early diagnosis and proper management are key. Despite its challenges, many people with lupus go on to live full and meaningful lives. Women with lupus can also have successful pregnancies with proper medical care. A knowledgeable and supportive rheumatologist is essential in managing the condition—choose one who listens, understands, and works closely with you on your treatment journey.
Vasculitis: Treatment, symptoms, causes, and types.
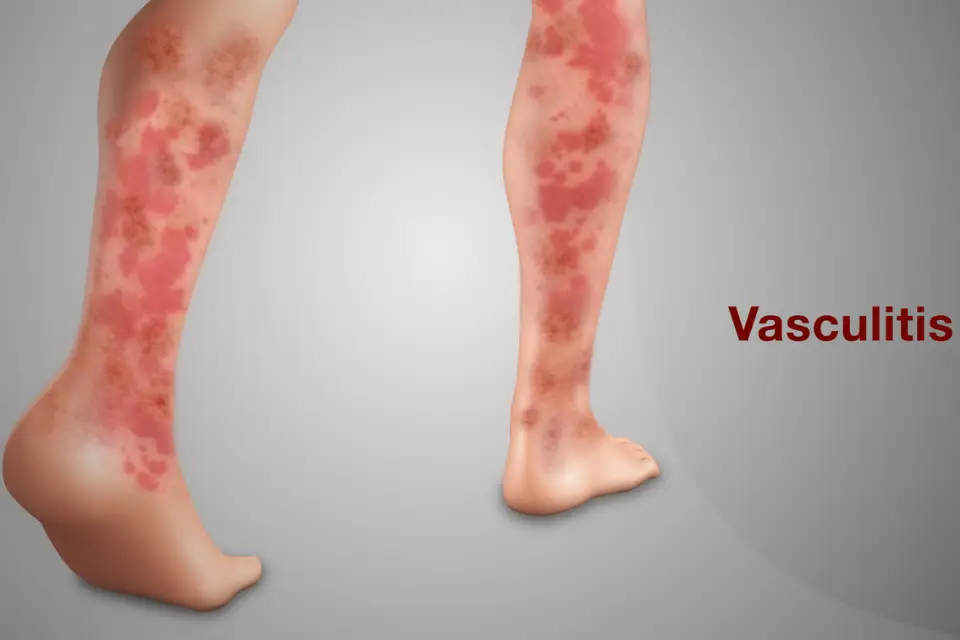
Vasculitis: What You Need to Know Vasculitis refers to a large group of diseases that cause inflammation of the blood vessels. It is also known as angiitis. This inflammation leads to changes in the walls of blood vessels, which may include scarring, weakening, narrowing, or thickening. These changes can occur in no particular sequence and may affect blood flow throughout the body. What Causes Vasculitis? Vasculitis occurs when the body’s immune system mistakenly attacks its own blood vessels. The exact cause is still not fully understood. However, known triggers include: Infections Certain cancers Immune system disorders Allergic reactions When blood vessels become inflamed, their walls may weaken, potentially leading to complications such as aneurysms (bulging of blood vessels). Types of Vasculitis There are two main categories of vasculitis: Primary vasculitis: Occurs without a known cause Secondary vasculitis: Develops as a result of another disease, such as rheumatoid arthritis or lupus Symptoms of Vasculitis Symptoms vary depending on which blood vessels are affected and which organs are involved. Common signs include: Fever Fatigue Weight loss and loss of appetite Joint pain Muscle pain Numbness or weakness Complications The severity of vasculitis depends on the type and extent of blood vessel involvement. A major complication is organ damage, caused by reduced oxygen and nutrient supply due to restricted blood flow. Although treatment can be effective, relapses may occur. In some cases, long-term management is required. Diagnosis Accurate diagnosis typically involves several tests, including: Blood tests Urine tests Tissue biopsy These help confirm inflammation and rule out other conditions. Treatment Treatment usually focuses on reducing inflammation and controlling the immune response. Common medications include: Corticosteroids (used to reduce inflammation) Drugs such as prednisone or methylprednisolone (Medrol) While effective, long-term use of steroids may lead to significant side effects, so careful medical supervision is essential. Summary Vasculitis has many potential causes, including infectious and immune-related conditions. Because it can affect multiple organs and systems, early diagnosis and treatment are critical. If you experience persistent symptoms, it is important to seek professional care from a rheumatologist as soon as possible.
Crohn’s disease: Symptoms, diet, causes, diagnosis, and more
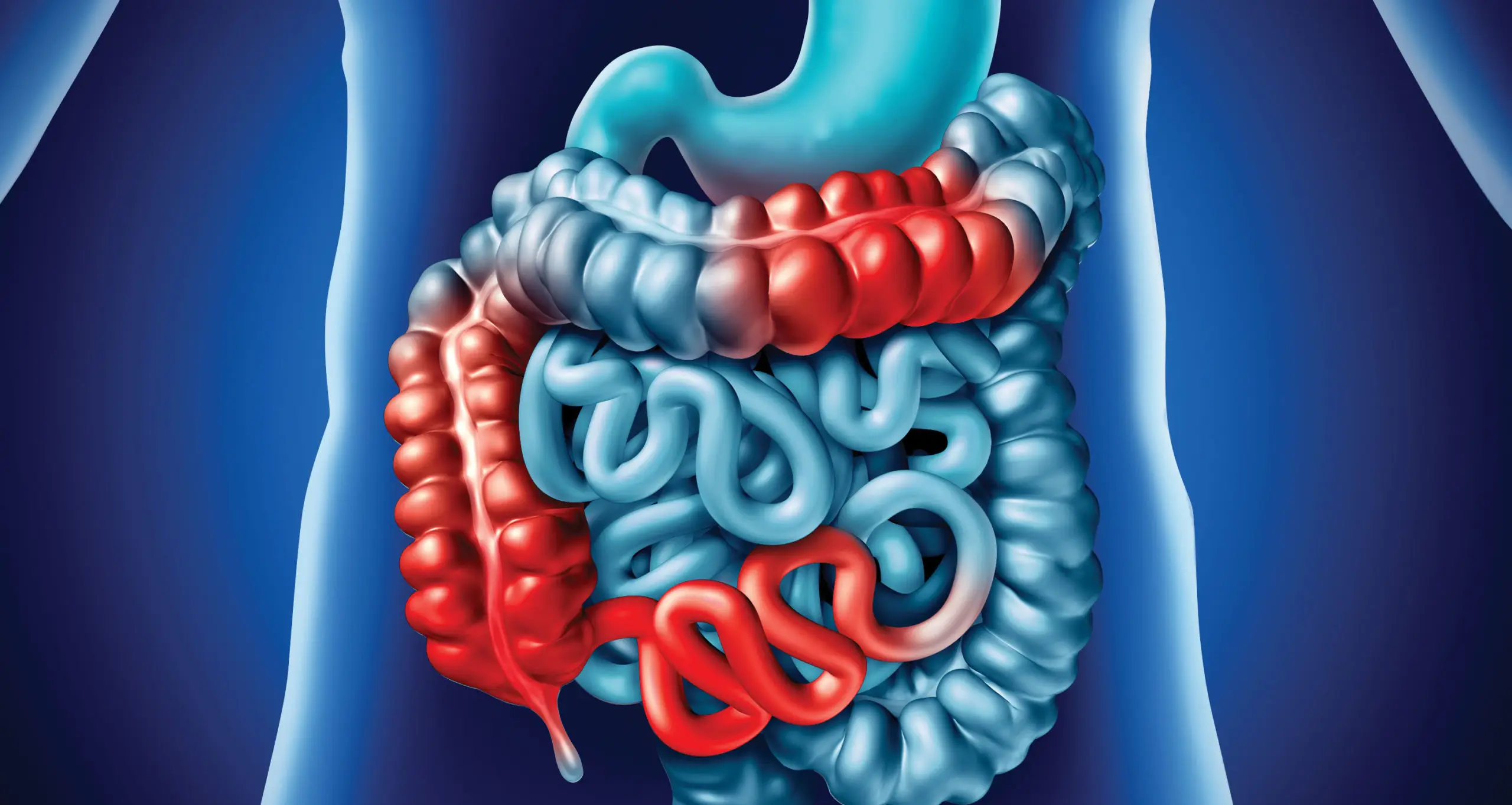
Crohn’s Disease: Causes, Treatment, and Management Crohn’s disease causes inflammation in parts of the digestive system. It can affect any area of the gastrointestinal tract, but it most commonly involves the small intestine and colon. Diagnosis and Causes Crohn’s disease is usually diagnosed only after other possible causes of symptoms have been ruled out. There is no single test that can confirm the condition. Instead, doctors use a combination of tests to support a diagnosis. Treatment The goals of Crohn’s disease treatment are to: Reduce inflammation that causes symptoms Improve long-term outcomes Prevent complications Achieve and maintain remission when possible Anti-inflammatory Medications Anti-inflammatory drugs are often the first step in treatment for inflammatory bowel disease (IBD). These may include: Corticosteroids These medications help reduce inflammation and control flare-ups. Surgery If diet changes, medications, or other treatments do not relieve symptoms, surgery may be recommended. Nearly half of people with Crohn’s disease will require at least one surgery in their lifetime. However, surgery does not cure the disease. During surgery: The damaged section of the digestive tract is removed Healthy sections are reconnected Fistulas may be closed Abscesses may be drained While surgery can provide relief, the benefits are often temporary, as Crohn’s disease may recur—frequently near the reconnected tissue. For best results, surgery is usually followed by medication to reduce the risk of recurrence. Diet and Lifestyle There is no clear evidence that diet causes inflammatory bowel disease. However, certain foods and drinks may worsen symptoms, especially during flare-ups. General dietary recommendations include: Limiting dairy products if they worsen symptoms Eating smaller, more frequent meals Drinking plenty of fluids Considering multivitamin supplements (under medical guidance) Consulting a registered dietitian for personalized advice Preparing for Your Doctor’s Visit Because consultation time is often limited, it helps to prepare a list of questions in advance. You may consider asking: What could be causing my symptoms? What tests will I need, and how should I prepare? Is this condition temporary or long-term? What treatment options are available, and which do you recommend? If I have Crohn’s disease, what is the risk of my child developing it? What follow-up tests will I need in the future? Summary Crohn’s disease is a long-term condition that requires ongoing management. Treatment is not a quick fix but a continuous process aimed at controlling symptoms and preventing complications. For best outcomes, it is important to work closely with a qualified specialist and follow a consistent treatment plan.
Ankylosing Spondylitis (AS): Symptoms, Causes & Treatment
What Is Ankylosing Spondylitis? Ankylosing spondylitis (AS) is a chronic inflammatory form of arthritis that primarily affects the spine. It causes pain, stiffness, and inflammation in the back and pelvis, and in severe cases, it can lead to reduced spinal mobility over time. People living with AS often experience periods of worsening symptoms known as flare-ups. Symptoms of Ankylosing Spondylitis Flares AS symptoms vary from person to person and often come and go in cycles. During flare-ups, common symptoms include: Lower back, hip, and pelvic pain Stiffness in the spine (especially in the morning) Rib cage, shoulder, knee, or joint pain Inflammation of tendons (enthesitis) Fatigue and low energy Fever during severe flares Anxiety or depression Other possible symptoms: Loss of appetite Digestive issues such as abdominal pain or loose stools Skin rashes in some cases What Causes Ankylosing Spondylitis? The exact cause of AS is not fully understood. However, research suggests a strong link to genetics—especially the HLA-B27 gene, which increases the risk of developing the condition. However, not everyone with the gene develops AS, and other environmental factors may also play a role. What Triggers AS Flares? The cause of flare-ups is not always clear, but several triggers may contribute: Physical stress or injury Illness or infections Poor sleep or fatigue High stress levels Lack of physical activity Even with careful management, flare-ups may still occur unpredictably. How Ankylosing Spondylitis Is Treated Treatment focuses on reducing inflammation, managing pain, and improving mobility. A rheumatologist typically designs a personalised treatment plan. Medications 1. NSAIDs (First-Line Treatment) Non-steroidal anti-inflammatory drugs such as: Ibuprofen Naproxen These help reduce pain and inflammation and are often the first treatment option. 2. Biologic Medications If NSAIDs are not effective, doctors may prescribe biologics that target the immune system to reduce inflammation more directly. Lifestyle & Physical Therapy Regular gentle exercise to maintain flexibility Stretching routines to reduce stiffness Physical therapy programs Posture correction exercises Supportive Therapies Massage therapy (when medically appropriate) Heat therapy for stiffness Stress management techniques Living With Ankylosing Spondylitis AS is a long-term condition, but symptoms can be managed effectively with proper care. Most patients benefit from: Early diagnosis Consistent medication use Active lifestyle habits Regular rheumatology follow-ups Can AS Flares Be Prevented? While flare-ups cannot always be prevented, their severity and frequency may be reduced by: Staying physically active Following prescribed treatment plans Avoiding known triggers Managing stress levels Prioritizing sleep and recovery Important Medical Note AS is a lifelong condition, and without proper treatment, it can lead to worsening stiffness and reduced spinal mobility. Early intervention is key to maintaining quality of life. Final Summary Ankylosing spondylitis is a chronic inflammatory condition that primarily affects the spine and joints. Although flare-ups are common, they can be managed effectively through: Medication Exercise Lifestyle adjustments Ongoing medical care With the right treatment plan, many patients live active and productive lives. 📍 Seek Specialist Care If you are experiencing persistent back pain, stiffness, or symptoms of AS, consult a rheumatology specialist for proper diagnosis and treatment. Piedmont Eastside Rheumatology📞 Contact a qualified rheumatologist today to develop a personalized treatment plan. ⚠️ Medical Disclaimer This article is for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.
What is Fibromyalgia
What Is Fibromyalgia? Fibromyalgia is a chronic pain disorder that affects the muscles, connective tissues, ligaments, and tendons. It causes widespread musculoskeletal pain, along with increased sensitivity to touch, pressure, and even normal sensations. According to specialists, fibromyalgia is linked to how the brain processes pain signals rather than physical damage in the body. “With fibromyalgia, we know there is an imbalance in the neurotransmitters that mediate pain,” explains Dr. Aloice Aluoch, a rheumatologist at Piedmont Eastside Rheumatology.“The balance between the brain’s feel-good and feel-bad chemicals is disrupted, making normal sensations feel painful.” Fibromyalgia Symptoms Fibromyalgia symptoms vary from person to person but commonly include: Widespread muscle and joint pain Extreme fatigue Sleep disturbances (including insomnia) Memory problems (“fibro fog”) Depression or mood changes Digestive issues such as irritable bowel syndrome (IBS) Heightened sensitivity to touch or pressure What Causes Fibromyalgia? The exact cause of fibromyalgia is not fully understood. However, it is believed to be related to how the brain and nervous system process pain signals. Possible triggers include: Physical or emotional stress Infections or illness Trauma or injury Hormonal changes Genetic predisposition Importantly, fibromyalgia is not an autoimmune disease and does not cause damage to joints, organs, or tissues. “Fibromyalgia does not damage your organs or joints,” says Dr. Aluoch.“It is not a deforming disease, but it can significantly affect quality of life due to persistent pain.” Who Is Most Affected? Fibromyalgia affects millions of people worldwide. According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases, approximately 5 million adults in the United States live with fibromyalgia. More than 80% of cases occur in women It is most commonly diagnosed in middle adulthood It often coexists with other chronic pain conditions How Is Fibromyalgia Treated? There is currently no cure for fibromyalgia, but symptoms can be effectively managed with the right approach. Treatment focuses on reducing pain, improving sleep, and enhancing daily function. Lifestyle & Therapy Options Doctors recommend lifestyle-based treatments such as: Regular aerobic exercise Aquatic therapy (water-based exercise) Yoga and stretching routines Stress management techniques Cognitive Behavioral Therapy (CBT) CBT and Mental Health Support Cognitive Behavioral Therapy helps patients: Reframe negative thoughts about pain Improve coping mechanisms Reduce stress-related symptom flare-ups Medications Depending on symptoms, doctors may prescribe: Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or aspirin Antidepressants to help regulate pain perception and improve sleep Other medications to manage chronic pain and fatigue Living With Fibromyalgia Fibromyalgia does not shorten life expectancy, but it can significantly affect daily living. With proper treatment, many patients are able to: Reduce pain levels Improve sleep quality Increase physical activity Improve mood and mental well-being Early diagnosis and a structured care plan are key to long-term management. When to See a Doctor You should consult a healthcare professional if you experience: Persistent widespread pain Chronic fatigue that does not improve with rest Sleep disturbances affecting daily life Memory or concentration problems A rheumatology specialist can help confirm diagnosis and develop a personalized treatment plan. Final Thoughts Fibromyalgia is a complex but manageable condition. While it can be frustrating and exhausting, the right combination of lifestyle changes, therapy, and medical support can significantly improve quality of life. 📍 Get Expert Help If you are experiencing chronic pain, fatigue, or fibromyalgia symptoms, consult a specialist for proper diagnosis and care. Piedmont Eastside Rheumatology📞 Book an appointment with a qualified physician today for evaluation and treatment options. ⚠️ Medical Disclaimer This content is for informational purposes only and should not replace professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment.