Osteoporosis: What You Need to Know
Osteoporosis weakens bones, making them more susceptible to sudden and unexpected fractures. It means you have reduced bone mass and strength.
The disease often progresses without symptoms or pain and is usually not discovered until weakened bones lead to fractures—most commonly in the hip, wrist, and spine.
What Causes Osteoporosis?
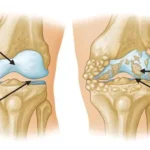
Your bones are made of living, growing tissue. The inside of healthy bones looks like a sponge. When osteoporosis occurs, the “holes” in that sponge grow larger and more numerous, weakening the bone.
Bone remodeling helps supply the body with needed calcium while keeping bones strong. However, after age 35, bone breakdown begins to occur faster than bone buildup, leading to a gradual loss of bone mass.
If you are experiencing menopause or already have osteoporosis, this breakdown happens even more rapidly.
Osteoporosis Symptoms
Osteoporosis is often called a “silent disease” because there are usually no visible symptoms. However, you should watch out for the following signs:
- Bone fractures
- Changes in posture (stooping or bending forward)
- Shortness of breath (due to reduced lung capacity from compressed discs)
- Loss of height (getting shorter by an inch or more)
- Lower back pain
Who Is at Risk?
Your risk of developing osteoporosis depends on several factors, including age, gender, and lifestyle:
- Risk increases with age (women over 50 are at the highest risk)
- Ethnicity plays a role (Caucasian and Asian women are more likely to develop osteoporosis, but African American and Hispanic women are also at risk)
- Family history can increase your chances
- Diets low in calcium and vitamin D contribute to bone loss
- Lifestyle habits like smoking and excessive alcohol use can increase risk
Osteoporosis Diagnosis
Your healthcare provider can assess your bone health before problems begin. A Bone Mineral Density (BMD) test is commonly used for diagnosis.
- Women over the age of 65 should have a BMD test
- Men over the age of 70 should also consider screening
Treatment for Osteoporosis
Treatment may include a combination of exercise, supplements, and medication.
Consider incorporating:
- Weight-bearing exercises
- Resistance training
- Balance exercises
Supplementation with calcium and vitamin D is often recommended to help prevent or manage osteoporosis.
Osteoporosis Medications
There is no single “best” medication for osteoporosis—the right treatment depends on your individual condition.
Common options include:
- Bisphosphonates (help prevent bone loss by slowing bone resorption)
- Biologics, such as Denosumab
Calcium Intake Guidelines
The recommended daily calcium intake is 1,000 mg to 1,200 mg, obtained through diet and/or supplements.
Taking more than this amount may increase the risk of:
- Kidney stones
- Calcium buildup in blood vessels
- Constipation
Always consult your healthcare provider before starting supplements.
Living with Osteoporosis
Managing osteoporosis involves making lifestyle adjustments:
- Get regular exercise
- Avoid excessive caffeine and alcohol
- Eat a balanced, nutrient-rich diet
- Reduce fall risks at home (use grab bars and stair railings)
Summary
You can still lead an active and fulfilling life with osteoporosis.
Always consult your rheumatologist if:
- You experience a fall
- You develop sudden or severe back pain
Working closely with a healthcare professional will help you manage the condition effectively and maintain your quality of life.