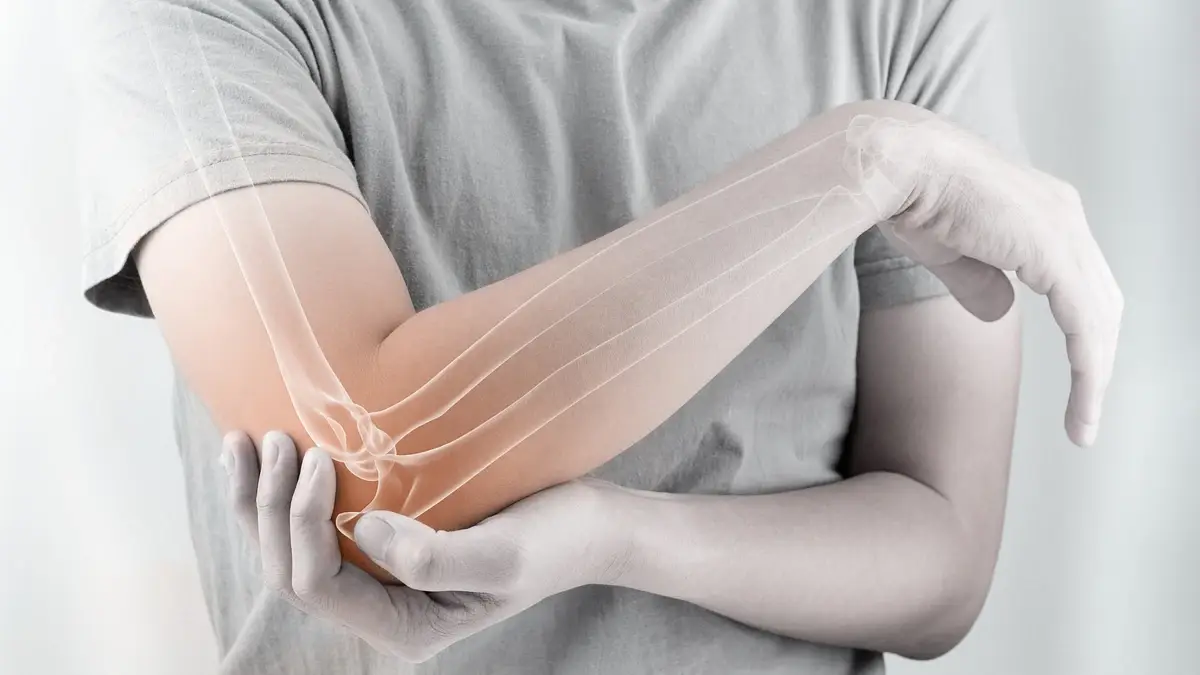
What Is Reactive Arthritis?
Reactive arthritis is a type of inflammatory arthritis that affects the joints, eyes, urinary tract (urethra), and skin.
It is often referred to as a post-infectious arthritis, meaning it develops in response to an infection elsewhere in the body.
The condition may develop gradually with periods of remission and recurrence, or it may appear suddenly with severe symptoms.
Reactive arthritis most commonly affects sexually active men between the ages of 20 and 40, and individuals living with HIV may have a higher risk.
What Causes Reactive Arthritis?
The exact cause of reactive arthritis is not fully understood. However, research suggests a strong link to genetic and infectious factors.
Key Causes and Triggers:
- Genetic predisposition, particularly the HLA-B27 marker
- Sexually transmitted infections such as Chlamydia trachomatis
- Gastrointestinal infections (from contaminated food or water)
Reactive arthritis typically develops after an infection, even when the infection itself has already resolved.
While practicing safe sex (e.g., condom use) can reduce the risk of certain infections, there is no guaranteed way to prevent reactive arthritis.
Reactive Arthritis Symptoms
Symptoms often appear 1 to 4 weeks after an infection and may affect different parts of the body.
Early Symptoms
- Painful urination
- Discharge from the penis (in men)
- Diarrhea (if intestinal infection is involved)
Joint Symptoms
- Pain and swelling in joints (knees, ankles, feet, hips)
- Inflammation in fingers and toes
- Usually affects one or a few joints at a time
Additional Symptoms
- Mouth ulcers
- Eye inflammation (redness, pain, blurred vision)
- Enthesitis (pain where tendons and ligaments attach to bone)
- Scaly skin rashes (especially on palms, soles, or scalp)
- Lower back pain due to sacroiliac joint involvement
How Is Reactive Arthritis Diagnosed?
Diagnosing reactive arthritis can be challenging because symptoms may not appear all at once.
There is no single test for the condition, but a rheumatologist may use:
- Medical history and symptom review
- Testing urethral discharge for sexually transmitted infections
- Stool tests to detect gastrointestinal infections
- Blood tests (including genetic markers like HLA-B27)
- Joint examination for inflammation
Reactive Arthritis Treatment
Treatment focuses on managing symptoms and addressing the underlying infection.
1. NSAIDs (Pain and Inflammation Relief)
Nonsteroidal anti-inflammatory drugs such as ibuprofen and naproxen are commonly used to reduce pain and swelling.
2. Antibiotics
If a bacterial infection (such as Chlamydia trachomatis) is identified, antibiotics are prescribed to treat the infection.
3. Steroids
Steroids may be used to treat:
- Joint inflammation
- Skin conditions
- Eye inflammation
4. Physical Therapy & Exercise
Patients with persistent symptoms may benefit from guided exercise programs to maintain joint mobility and strength.
Complications of Reactive Arthritis
Although many people recover fully, some may experience complications, including:
- Chronic arthritis
- Recurring symptoms
- Inflammation of the heart muscle
- Eye complications such as glaucoma
Prognosis: What to Expect
The outlook for reactive arthritis varies from person to person.
- Most people recover within 3 to 4 months
- About 50% may experience recurrence over time
- A small number may develop long-term or chronic symptoms
Early diagnosis and treatment significantly improve outcomes.
Living With Reactive Arthritis
Managing reactive arthritis involves:
- Seeking early medical care after infections
- Practicing safe sex to reduce STI risk
- Following prescribed treatment plans
- Staying physically active to support joint health
- Regular follow-ups with a rheumatologist
Summary
Reactive arthritis is an inflammatory condition triggered by infections, affecting joints and other parts of the body.
While it can be uncomfortable and sometimes recurrent, most people recover fully with proper treatment and care.
⚠️ Medical Disclaimer
This content is for informational purposes only and does not substitute professional medical advice. Always consult a qualified healthcare provider or rheumatologist for proper diagnosis and treatment.